Welcome to Space Race, where we explore the impact of breakthroughs in science research on the 21st century. Subscribe for weekly breakdowns of the scientific breakthroughs that will shape the future.
In this week’s newsletter we discuss mRNA vaccines. Made famous by their rapid deployment during the COVID-19 pandemic, mRNA vaccines represent a multi-decade triumph of science. We’ll break down what mRNA is, its role in vaccines, and the advantages of mRNA vaccines vs traditional vaccines. We’ll also discuss the technical challenges that were overcome to make these vaccines, and how mRNA technology could lead to an era of personalised vaccines.
Crises often give rise to incredible innovation, and by any yardstick COVID-19 is the most serious crisis in generations. In the span of less than two years, it has snowballed from an odd curiosity to a global pandemic claiming millions of lives. However, in an even smaller timespan, scientists have innovated and produced vaccines that can successfully protect against the new virus. Scarcely a year after the first case, humanity already had a weapon against its new biological enemy. This record time was only possible due to the invention of mRNA vaccines, which signals the beginning of a new era in vaccinology.
What is mRNA?
Most of us are familiar with DNA, the molecule that sits in the nuclei of our cells and acts as the blueprint for all biological function. Every organ in our body is made up of proteins, and DNA contains the instructions which the cell uses to make those proteins. This information is stored in the ordering of four genetic bases: Adenine (A), Thymine (T), Cytosine (C), and Guanine (G). The different orderings of these bases in DNA sequences correspond to different proteins.
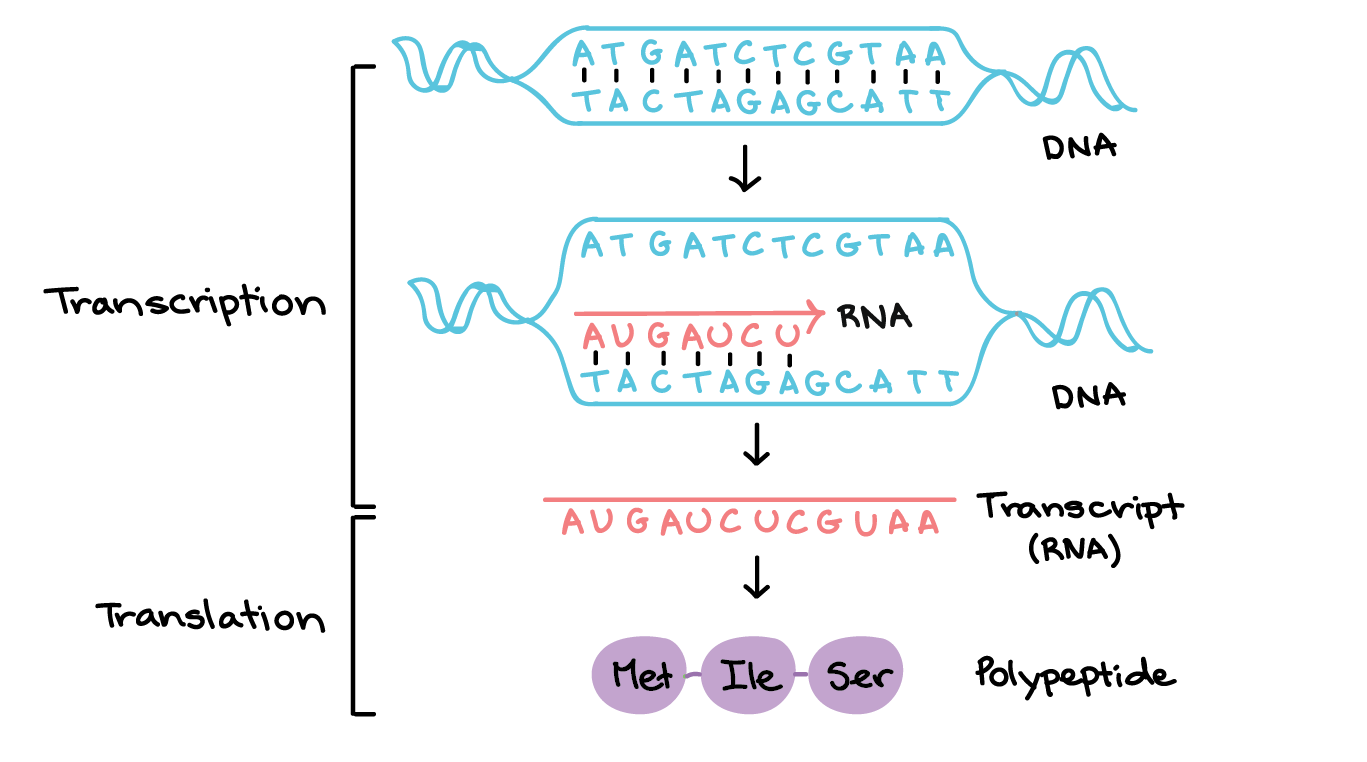
mRNA is a very important supporting character in the process of protein synthesis. While DNA is the genetic blueprint for all biological function, mRNA is the means by which that blueprint is translated into actual proteins. More precisely, mRNA is created from a particular segment of DNA in a process known as transcription. The DNA in the nucleus is unzipped by special enzymes and mRNA is created by matching bases to one side of the double helix. This way, we the mRNA copies ("transcribes”) the information stored in the DNA.
Once transcribed, the new mRNA leaves the nucleus and goes to a cell organelle called a ribosome. The ribosome reads (“translates”) the mRNA and makes the proteins that it codes for.
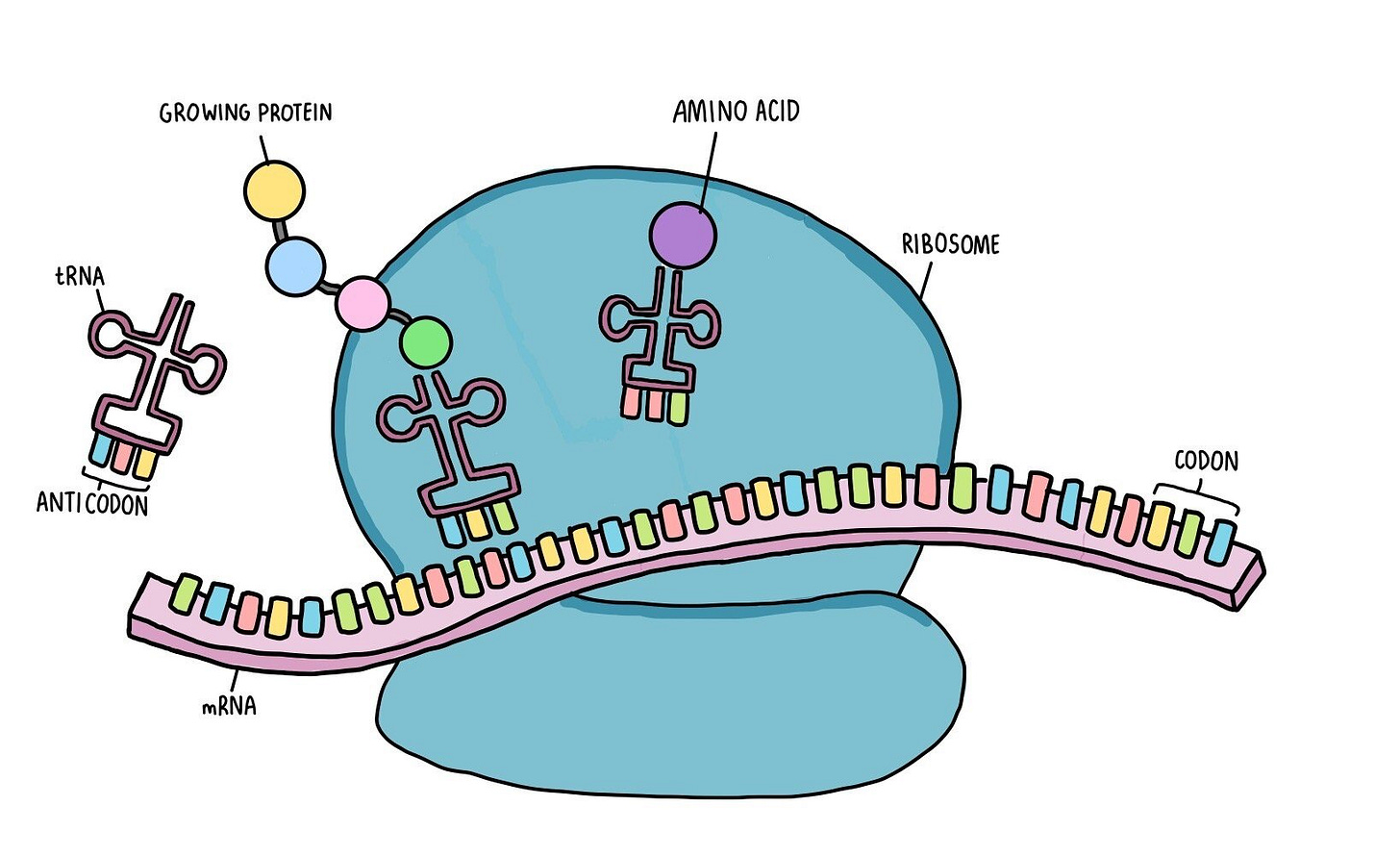
Traditional Vaccines
Before mRNA vaccines, let’s remind ourselves of how traditional vaccines work. The role of vaccines is to safely expose our immune systems to an antigen, which is a protein from a virus (or other pathogen) that is harmless. Through this harmless exposure, the immune system can learn to recognise and eliminate this foreign antigen, remembering it in the process. Now, in the event of real exposure, the immune system can quickly recognise and destroy the actual virus before it can do any harm. We have become immunised.
An example of such an antigen is the spike protein on the surface of the COVID-19 virus. While it plays a role in helping the virus bind to healthy cells, it doesn’t cause the actual symptoms or infection. By itself, the spike protein is harmless.
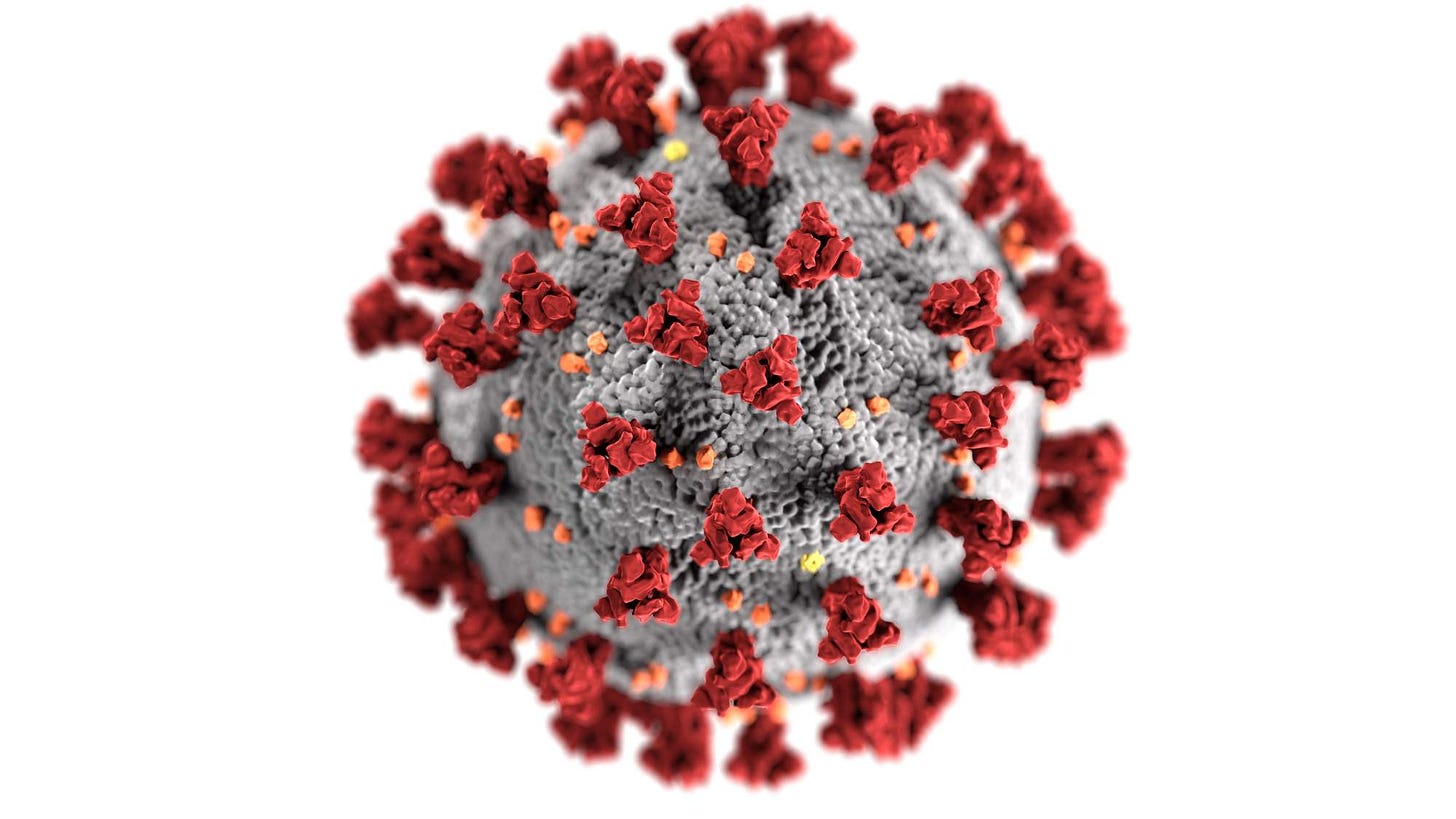
Traditional vaccines rely on various methods to achieve this harmless exposure. The most common are:
Inactivated virus vaccines: these use an “inactivated” (already killed) version of the virus to build immunity. An example is the polio vaccine, which has been phenomenally successful in eradicating polio from much of the world.
Weakened virus vaccines: these use live but artificially weakened viral samples. The MMR vaccine against measles, mumps, and rubella is an example of this, as is the first vaccine ever invented against smallpox in 1796.
Subunit vaccines: instead of a full virus, these vaccines use specific harmless proteins from the virus for exposure. The first subunit vaccine approved in the US was for Hepatitis B in 1981, and it used the virus’ HBsAg surface protein.
Viral vector vaccines: these vaccines work by transferring segments of viral RNA that code for harmless antigens into human cells. When ribosomes read the viral RNA, they will produce the harmless antigens which will train the immune system. As the name suggests, viral vector vaccines cleverly use viruses themselves as the delivery mechanism for the RNA payload into the cell. Of the main COVID-19 vaccines, Oxford-AstraZeneca, Sputnik V, and Johnson & Johnson all use viral vector technology.
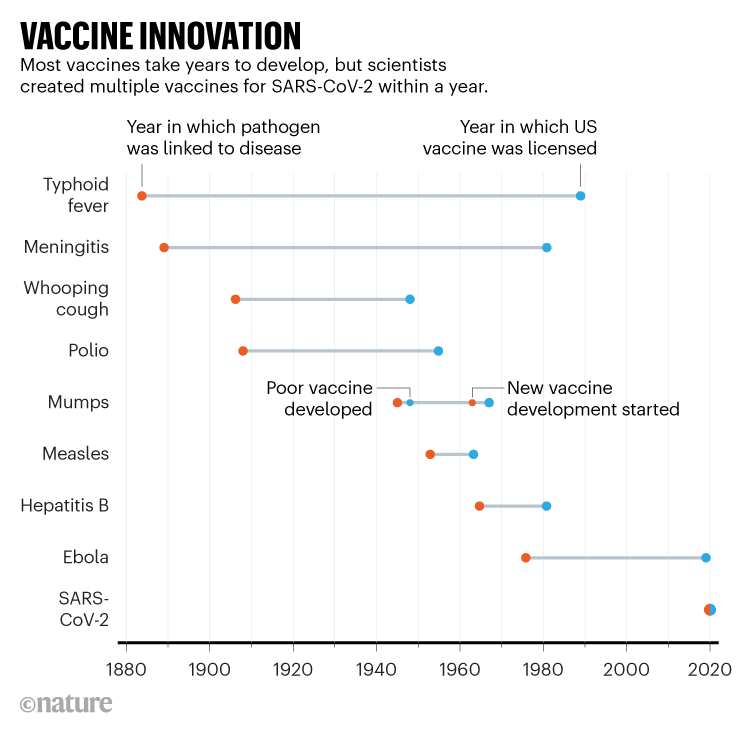
As shown by the examples, all of these techniques have produced extremely successful vaccines. However, many of these approaches take a very long amount of time to produce safe and effective vaccines. The measles vaccine took almost 10 years to make because it took time to grow the measles virus. This is not as much of a problem for viral vector vaccines, as the quick development of the three COVID-19 vaccines shows, but they have other issues. One difficulty is selecting the right viral vector that is harmless to the body but at the same time won’t get destroyed by the immune system before it can transfer the viral RNA.

mRNA Vaccines
Like viral vector vaccines, mRNA vaccines aim to inject RNA into human cells so that they produce antigens. For the Moderna and Pfizer-BioNTech vaccines, the harmless antigen is the spike protein. The main difference is that mRNA vaccines don’t use a virus to deliver RNA and inject it directly into cells. Once inside, the RNA is naturally broken down by the body, leaving no trace of the vaccine.
The key advantage of direct RNA delivery is that it makes these vaccines incredibly easy to make and very flexible. All that’s needed is the genetic sequence of the target viral RNA segment. With modern genetic sequencing technology, this has become much easier. The spike protein of the original Wuhan variant was sequenced as early as January 2020. Two days after the initial release of the sequence by Chinese authorities, Moderna had developed mRNA sequence mRNA-1273 for its vaccine. Subsequent trials demonstrated that both Moderna and Pfizer-BioNTech’s mRNA vaccines were around 90% effective against the initial COVID variant, an incredible figure for the first ever mRNA vaccines.
However, due to ineffective global vaccine distribution, the COVID-19 virus has also been able to evolve against our defenses. This gave rise to the new omicron variant, whose spike protein sequence variant has some differences from the original sequence. These genetic mutations mean that mRNA vaccines are not as effective against omicron as they are against the initial COVID-19 variants - although they are still highly effective at protecting against severe disease!
This is where the flexibility and speed of mRNA vaccines truly shines. If necessary, omicron specific mRNA vaccines could be developed just as quickly as the original variant vaccines. Pfizer-BioNTech and Moderna both claim they could have omicron boosters ready by March 2022, just a few months after omicron was first identified.
Challenges of Making an mRNA Vaccine
However, mRNA technology didn’t simply drop out of the void just in our hour of need. The development of mRNA vaccines relied on solving some difficult technical challenges that had bogged the field since its inception in the late 1980s.
The first challenge stems from the fact that free-floating RNA outside cells is quickly targeted and destroyed by the body. Synthetic RNA was found to activate toll-like receptors, which are a series of sensors in the immune system that activate in response to foreign material in the body. When this happened, the immune system would quickly destroy the mRNA before it could do anything useful, making any such vaccine useless. Karikó et al. were able to show that by making a slight chemical modification of the U mRNA base, they could prevent the immune system from attacking the mRNA fragment.
The second technical challenge was that mRNA molecules cannot get through the membrane that surrounds cells. This problem was eventually solved by wrapping mRNA payloads in tiny bubbles of fat molecules called lipids. These lipid nanoparticles, or LNPs, both protect the mRNA payload and enable it to enter cells through the process of endocytosis, when the cell engulfs the LNP surrounding the mRNA. Once inside, the LNP breaks down and the mRNA can be read by the ribosomes.
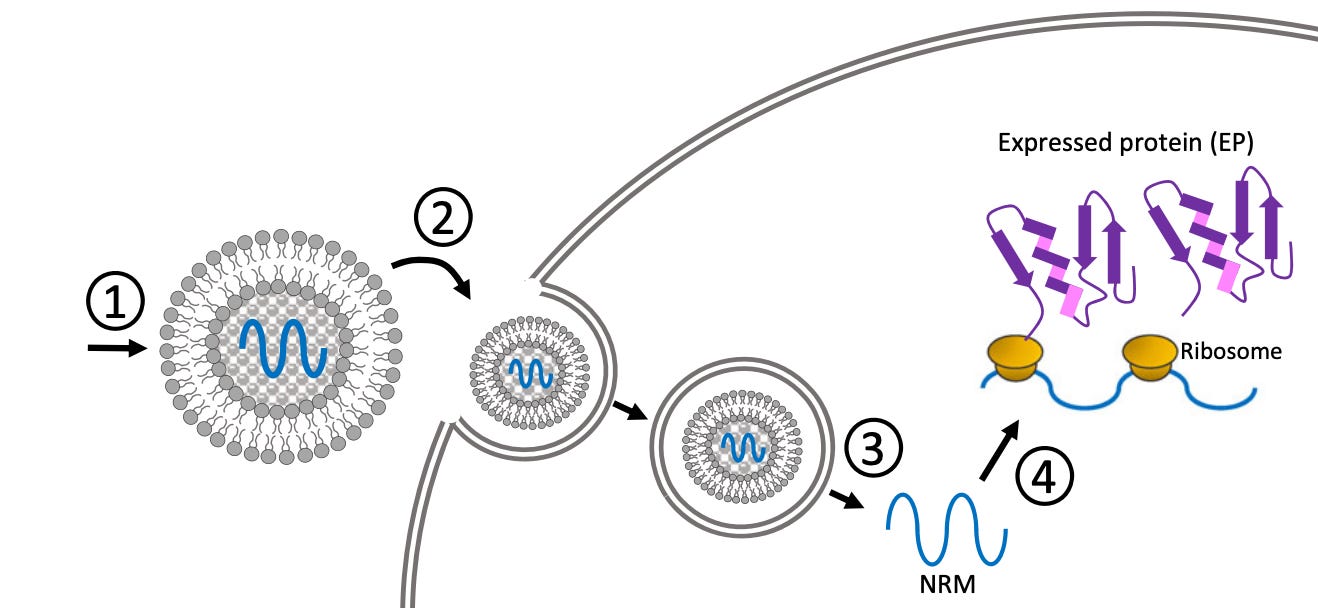
LNP techniques have been studied since the early 1990s, and continually improved since then. The first LNP based RNA drug targeting a rare genetic disorder was approved by the FDA in 2018, which was a critical step in validating LNP techniques and RNA based medicine.
Future Prospects
Now that mRNA technology has proven itself in the toughest of circumstances, it is natural to wonder what might be next. One reason why mRNA technology is so powerful is because it provides a versatile platform for vaccine development. By simply swapping in one genetic sequence for another, the same manufacturing process can be used to produce vaccines for many diseases at scale. Currently, researchers are exploring possibilities for mRNA vaccines for influenza, Zika, HIV, and even cancer.
The prospects for personalised mRNA vaccines are particularly interesting. One example of this is using vaccines to support immunotherapy, where the body’s immune system is stimulated to destroy cancer cells. Although it sounds simple in theory, treating cancer like this can be very difficult in practice. A huge problem is the fact that many patients’ cancers have a weak or nonexistent response to immunotherapy.
To counter this, companies such as Moderna and BioNTech are developing personalised mRNA-based cancer vaccines. This relies on the fact that cancer cells have mutations in their DNA that produce proteins called neoepitopes. These are recognisable targets for the immune system and can initiate an immune response. To make the vaccine, we first sequence the patient’s cancerous DNA to identify the neoepitopes it produces which will have the strongest immune response. Once we have the sequences, we can make mRNA that codes for these proteins and inject the vaccine. Now the body’s cells can produce even more of the neoepitopes made by the patient’s own cancer cells, which in turn has a greater chance of activating an immune response and destroying the cancer cells. The flexibility of mRNA technology in this case allows us to rapidly make vaccines customised to individual patients’ cancer mutations.
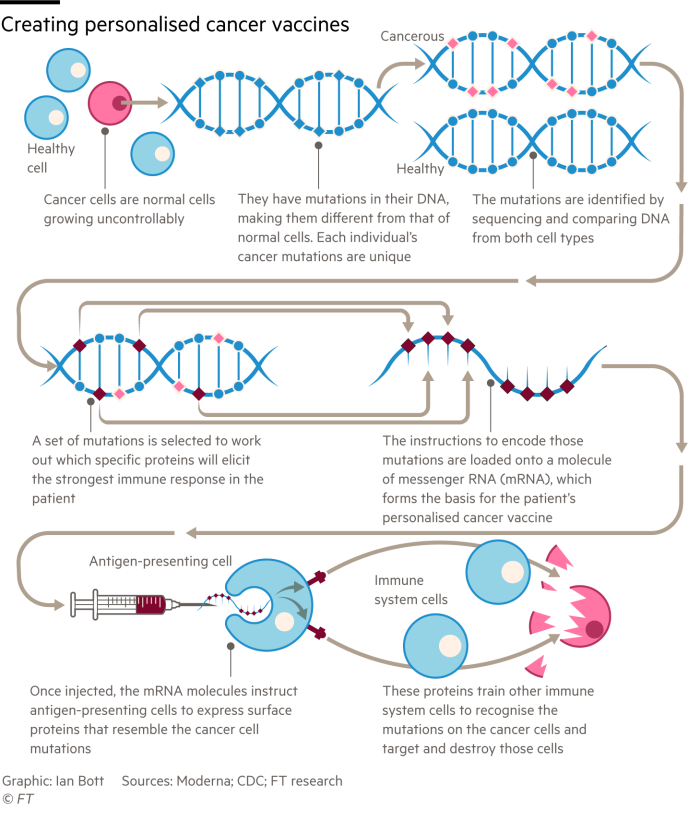
Crises breed innovation, and the COVID-19 crisis was the stage that allowed mRNA technology to shine. After decades of fighting against difficult technical challenges, scientists were finally able to directly inject mRNA into the body, paving the way for mRNA vaccines. Since they deliver genetic payloads directly to our cells without the need for an intermediate vector like a virus, mRNA vaccines offer unmatched flexibility and speed compared with traditional vaccines. To engineer the mRNA sequence, a genetic sequence from the pathogen in question is all that is needed. This is why these vaccines were produced in record time, turning the tide in the fight against COVID-19.
More broadly, mRNA technology offers an incredibly versatile platform for vaccines for all types of diseases. All that’s required is replacing one pathogenic sequence with another, in stark contrast with traditional vaccines which usually need specialised production pipelines. Complementing this generalisation at the production level is the ability to personalise vaccines at the patient level, as shown by the possibility of mRNA vaccines custom made for individual cancer patients. Due to these advantages, mRNA technology is set to usher in a new era of vaccines which are readily available yet exquisitely personalised for a new level of care.






I really like how you discussed the timeline of vaccine innovation. I never realized how long the process was in the past to get vaccines out to others. I didn't even register that the Ebola vaccine took as long as it did to be available to the public.
Another portion of your article that I liked was when you presented and theorized where mRNA vaccines can take us next. Cancer and HIV mRNA vaccines - wow. I feel like I have done myself a massive disservice in not keeping up with science and all the developments that have been made!